People with Disabilities have the right to Good health too

Put simply; the disabled population is one whose health care needs are not being met.
Keep in mind that people with disabilities often live shorter lives (nearly 15-20 years less than the general population) and when we combine the ‘health inequality’ challenges these persons face, we reason that they are more likely to die of preventable causes.
Take for instance; people with autism and Down’s syndrome may be unable to tell a doctor when they feel unwell, they are less likely to have their weight checked (in turn, they report higher rates of obesity); they will also eat poorly and practice physical inactivity. Further; deaf people are more likely to have undiagnosed high blood pressure, undiagnosed diabetes, high cholesterol, and cardiovascular diseases than the average ‘hearing population’, they may even take medications without appropriate clinical justification (over-medicate) while struggling to make themselves understood.
A 2015 survey showed that between 35% and 50% of people with serious disabilities (living in developed countries), and between 65% and 80% of people with serious disabilities (living in developing countries) – received no treatment in 2014. You should take note that these persons also report seeking more health care than people without disabilities, despite the fact that they encounter a wide range of barriers when they attempt to access health care.
So why do people with significant disabilities have less access to health care services? Why are health care services not designed with their needs in mind? Why do health prevention activities seldom target these people? Shall we continue to ignore their medical needs?
Read on; because in this article, we’ll discuss the barriers they face and how health outcomes can be improved for people with disabilities.
First, we’ll look at the barriers to health care of people with disabilities – they include;
- Prohibitive costs:
In low-income countries, people with disabilities do not receive needed health care due to affordability of health services, from drugs to procedures and hospitalization – they are unable to afford these services which are a major financial drain to anyone, anywhere.
- Limited availability of services:
When people with disabilities are faced with lack of appropriate services, this becomes a significant barrier. For example; access to health services is limited or difficult in many rural communities.
- Physical barriers:
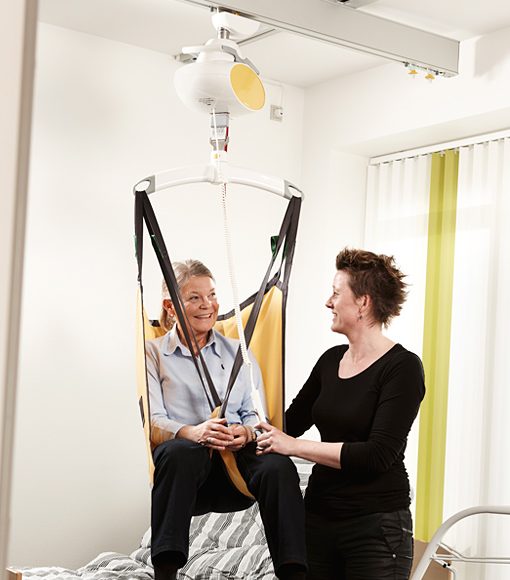
From technological problems to noise, inaccessible medical equipments, narrow doorways, inadequate bathroom facilities, and other interior workspace design problems – all these create barriers to health care facilities. For example; patient transfers may be difficult without a ceiling lift system.
- Inadequate skills, knowledge and inappropriate attitude of health workers:
Persons with disabilities often experience finding healthcare provider skills not good enough to meet their needs, being treated badly, and being denied care in general.
Now, we’ll focus on how Governments can address these barriers to health care with services that are progressive and high quality.
- Policy and legalization:
By assessing policies, identifying priorities, and establishing health care standards related to care of people with disabilities, health inequalities can be drastically reduced.
- Financing:
People with disabilities should benefit equally from public health care programs, they should be covered and also be able to afford the premiums.
- Service delivery:
Provide a range of adjustments to facilitate access to health care services. In addition; people with disabilities should be empowered to maximize their health by providing them basic information and training.
- Data and research:
Basically; research on the needs and barriers for people with disabilities can (and should) be conducted.